The five stages change model
Behavioural support is an important part of any smoking cessation attempt and should be recommended to all individuals who intend to stop smoking.Introduction
If we consider that 40% of nicotine users make a cessation attempt annually, but only 4-6% manage to maintain abstinence, a mere 2% of nicotine users reach full cessation per annum.
One third of successful cessation attempts necessitate either medical or psychological therapy to result in a successful outcome.
Practitioners must be supportive and understanding of the patient’s wishes, alongside understanding that utilisation of the ‘3A’s,’ approach of brief cessation advice can offer some benefit. Understanding the ‘Stages of Change,’ model allows healthcare practitioners to intervene appropriately.
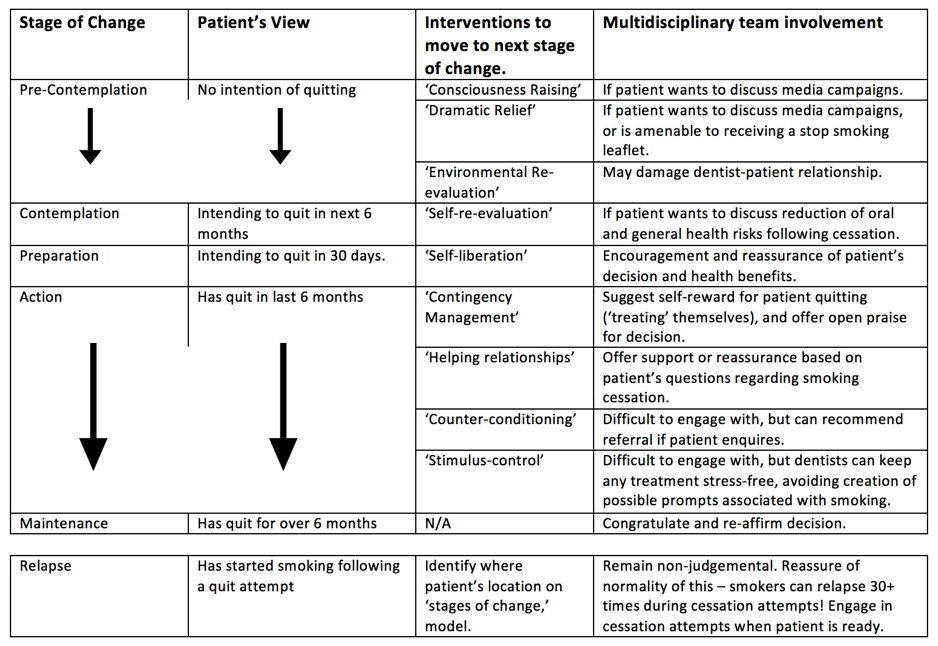
The suggestion that smoking cessation could be split into five different stages was first described by Prochaska and DiClemente (1983), with potential interventions to progress individuals through the 5 stages listed in the table below.

5 Stages of Change Model
Pre-Contemplation
This is the stage where an individual has no intention to alter their habit in the near term, which is normally deemed to be within the next six months. In this stage, individuals are often defensive, avoiding thinking or talking about their high-risk behaviour.
They may not be considering change because they are demoralised at previous quit attempts, do not understand the consequences of their actions or believe the consequences are insignificant. Simply put, at this stage the pros of smoking are outweighing the cons of smoking for the individual. To progress from this stage, an individual must accept their actions are problematic and potential harmful to themselves and others
Contemplation
Whilst in this stage, the individual will be aware of the inherent risks of their actions, but is ultimately unwilling to change. Whilst in this stage, the individual is in a state of flux, weighing up the pros and cons.
Preparation
Preparation
In this stage, the individual plans to make the change away from their harmful behaviour within one month. This stage of change usually consists of individuals who have attempted to change from their ‘at risk’ behaviour in the last 12 months, but have relapsed and are still engaging in the activity.
The individual must decide on a strategy which results in the desired outcome. As many in this stage have attempted to change their behaviour once (or more times) before, they will often adopt a different method of progressing into the action phase.
Action
Action
In this stage, the individual has made the move to alter their harmful behaviour within the last 6 months. During this stage, the individual will both receive the greatest plaudits for their efforts from others, but also find this stage the most difficult due to withdrawal symptoms.
The individual must remain in the action state until they move towards a state of ‘self-efficacy,’ and this is stronger than their temptation to revert to the problem behaviour.
Maintenance
It is shown that a majority of relapses from maintenance state happen in the presence of other smokers and to be successful individuals tend to avoid social situations with other smokers. Those who never smoke again remain in the maintenance stage.
For an addict, there is always a potential of relapse.

Relapse
To reverse relapse, it is important for the individual to remember why they quit in the first place. Relapses are a normal part of the change process and those that have relapsed should be reassured as such.
An individual may relapse as many as 30 times during their attempt to stop smoking.
How to interact with a smoker
Bibliography & Further Reading
Bandura A. Self-efficacy mechanism in human agency. American psychologist. 1982 Feb;37(2):122.
Center for Disease Control and Prevention. Cigarette smoking among adults—United States, 1998. Morb Mortal Wkly Rep. 2000;49:881–4.
Chaiton M, Diemert L, Cohen JE, Bondy SJ, Selby P, Philipneri A, Schwartz R. Estimating the number of quit attempts it takes to quit smoking successfully in a longitudinal cohort of smokers. BMJ Open. 2016 Jun 1;6(6):e011045.
Cohen S, Lichtenstein E, Prochaska JO, et al. Debunking myths about self-quitting. Am Psychol. 1989;44:1355–65.
Cornuz J, Willi C. Nonpharmacological smoking cessation interventions in clinical practice. European respiratory review. 2008 Dec 1;17(110):187-91.
Ferguson SG, Frandsen M, Dunbar MS, Shiffman S. Gender and stimulus control of smoking behavior. Nicotine & Tobacco Research. 2015 Apr 1;17(4):431-7.
Fiore MC, Jaen CR, Baker TB, Bailey WC, Benowitz N, Curry SJ. Treating Tobacco Use and Dependence: 2008 Update. Clinical Practice Guideline. Rockville MD: US Department of Health and Human Services, Public Health Service; 2008.
Foss R. Personality, social influence and cigarette smoking. J Health Soc Behav 1973; 14(3):279–286.
Higgins ST, Petry NM. Contingency management incentives for sobriety. Alcohol research & health. 1999 Mar 22;23(2):122-.
Hughes JR, Burns DM. Population Based Smoking Cessation. Bethesda, MD: National Cancer Institute;; 2001. Impact of medications on smoking cessation; pp. 155–64. Proceedings of a Conference on What Works to Influence Cessation in the General Population, Smoking and Tobacco Control, Monograph No. 12.
Hughes JR. Four beliefs that may impede progress in the treatment of smoking. Tobacco Control. 1999 Sep 1;8(3):323-6.
Humphreys K, Mankowski ES, Moos RH, Finney JW. Do enhanced friendship networks and active coping mediate the effect of self-help groups on substance abuse?. Annals of Behavioral Medicine. 1999 Mar 1;21(1):54-60.
Lancaster T, Stead LF. Individual behavioural counselling for smoking cessation. The Cochrane Library. 2005 Jan 1.
Lenio JA. Analysis of the Transtheoretical Model of behavior change. Journal of Student research. 2006;5:73-87.
Levesque DA, Cummins CO, Prochaska JM, Prochaska JO. Stage of Change for Making an Informed Decision about Medicare Health Plans. Health Services Research. 2006 Aug;41(4 Pt 1):1372.
Lindhe Söderlund, L. Motivational Interviewing in Theory and Practice. Digitala Vetenskapliga Arkivet 2010; 1198(): . http://www.diva-portal.org/smash/record.jsf?pid=diva2%3A356212&dswid=-6521 (accessed 10/11/16).
McNeill A., Raw M., Bauld L., Coleman T. (Guest Editors). Smoking treatment services in England: implementation and outcomes. Addiction 2005; 100
Moore M, Highstein G, Tschannen-Moran B, Silverio G. Coaching behavior change. Coaching: Psychology manual. 2010:33-51.
Morphett K, Partridge B, Gartner C, Carter A, Hall W. Why don’t smokers want help to quit? A qualitative study of smokers’ attitudes towards assisted vs. unassisted quitting. International journal of environmental research and public health. 2015 Jun 10;12(6):6591-607.
Orleans CT, Schoenbach VJ, Wagner EH, Quade D, Salmon MA, Pearson DC, Fiedler J, Porter CQ, Kaplan BH. Self-help quit smoking interventions: effects of self-help materials, social support instructions, and telephone counseling. Journal of consulting and clinical psychology. 1991 Jun;59(3):439.
Patten S, Vollman A, Thurston W. The utility of the transtheoretical model of behavior change for HIV risk reduction in injection drug users. Journal of the Association of Nurses in AIDS Care. 2000 Feb 29;11(1):57-66.
Prochaska JO, DiClemente CC, Norcross JC. In search of how people change: applications to addictive behaviors. American psychologist. 1992 Sep;47(9):1102.
Prochaska JO, DiClemente CC. Stages and Processes of Self-Change of Smoking: Toward an Integrative Model of Change. Journal of Consulting and Clinical Psychology. 1983 Jun;51(3):390-95.
Prochaska JO, DiClemente CC. The transtheoretical approach. Handbook of psychotherapy integration. 2005 Feb 24;2:147-71.
PrOchaska JO, Prochaska JM. Behavior change. Population health: creating a culture of wellness. 2010 Oct 25.
Prochaska JO, Velicer WF. The transtheoretical model of health behavior change. American journal of health promotion. 1997 Sep 1;12(1):38-48.
Prochaska JO. Transtheoretical model of behavior change. InEncyclopedia of behavioral medicine 2013 (pp. 1997-2000). Springer New York.
Raw M, McNeill A, Murray R. Case studies of tobacco dependence treatment in Brazil, England, India, South Africa and Uruguay. Addiction. 2010 Oct 1;105(10):1721-8.
Roddy E, Antoniak M, Britton J, Molyneux A, Lewis S. Barriers and motivators to gaining access to smoking cessation services amongst deprived smokers–a qualitative study. BMC Health Services Research. 2006 Nov 6;6(1):1.
Royal College of Physicians. Nicotine Addition in Britain. London, United Kingdom: Royal College of Physicians; 2000.
Siqueira LM, Rolnitzky LM, Rickert VI. Smoking cessation in adolescents: the role of nicotine dependence, stress, and coping methods. Archives of pediatrics & adolescent medicine. 2001 Apr 1;155(4):489-95.
Smith AL, Carter SM, Chapman S, Dunlop SM, Freeman B. Why do smokers try to quit without medication or counselling? A qualitative study with ex-smokers. BMJ open. 2015 Apr 1;5(4):e007301.
Stead LF, Lancaster T. Group behaviour therapy programmes for smoking cessation. Cochrane Database Syst Rev. 2005 Apr 18;2(2).
Taylor T, Lader D, Bryant A, Keyse L, Joloza MT. Smoking-related Behaviours And Attitudes 2005. London, United Kingdom: Office for National Statistics; 2005.
Tseng YH, Jaw SP, Lin TL, Ho CC. Exercise motivation and processes of change in community-dwelling older persons. Journal of Nursing Research. 2003 Dec 1;11(4):269-76.
U.S. Department of Health and Human Services (USDHHS). Reducing the health consequences of smoking: 25 years of progress. A report of the Surgeon General. Rockville (MD): U.S. Department of Health and Human Services, Centers for Disease Control, Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health; 1989. DHHS Pub. no. CDC 89-8411
Uppal N, Shahab L, Britton J, Ratschen E. The forgotten smoker: a qualitative study of attitudes towards smoking, quitting, and tobacco control policies among continuing smokers. BMC public health. 2013 May 3;13(1):1.
Velicer WF, Prochaska JO, Fava JL, Norman GJ, Redding CA. Smoking cessation and stress management: applications of the transtheoretical model. Homeostasis. 1998;38:216-33.
Venters MH, Solberg LI, Kottke TE, Brekke M, Pechacek TF, Grimm RH, Jr. Smoking patterns among social contacts of smokers, ex-smokers, and never smokers: the Doctors Helping Smokers Study. Prev Med 1987; 16(5):626–635.
Zimmerman GL, Olsen CG, Bosworth MF. A’stages of change’approach to helping patients change behavior. American family physician. 2000 Mar 1;61(5):1409.
Photos
Incense smoke (4) by losvizzero. Available at https://www.flickr.com/photos/folcobanfi/779572643/in/photolist-2bTvMD-7LpFkX-wxYDHW-apKcq5-4z9LEf-51mjSz-d34hh3-jpJPNp-4z9NVY-4z5xaM-PA1fhn-5ZUDyw-Ba5ox-4z9LTQ-itvTyk-dugc8b-nRxSnx-feQRqR-615wyM-bkCZoR-7CPT5c-4GsjjS-82Hb92-pzhfxD-4z5wrn-4Mrq6v-mw9vPZ-oWEA5t-4z9Kkf-2vVkpu-dxfnkW-pSg4d2-Sq7YAw-5LDsTX-8qfzJA-2bTwa4-eg3hB-4jbxjT-7QJ4xL-9DvemK-8KGdUq-7TKDf5-p6CrVD-6meTqN-agyBXN-oMWnEK-ijBdaF-CqJyt-dPiCM2-ThKCrH Licensed under CC BY-NC-ND 2.0
Change by Lee Jing Xi. Available at https://www.flickr.com/photos/jinx_1303/2973888147/in/photolist-5wMXkz-dhXVe4-dijMPN-4CruYx-qm3sT-7hi9oa-4BrZcd-4DZJzU-5UdnQF-cnz2vq-8eHE6w-JZXJ7-48uEZ-7zmw8k-4HRkPv-BmgGd-nyNtB-e2EaPE-5vRXVk-5G9zSv-5Au5JJ-5CHqbA-dyp4kq-8fmKCS-2qqWSF-6Niqwn-BmgGS-BmgFH-ovriCL-7eqWu-6BH6Kq-du8yPb-6puo57-99vLQv-7hkdvW-T5x8Th-8YENrX-6aKEQv-e8uDwc-dcZaG7-69cbLV-qxXmxV-oD5tjD-bwGbQX-bWXcoF-61hvET-9G8ERM-4oPJUQ-bygTHu-JvCYcH Licensed under CC BY-NC-ND 2.0
Glowing Ribbons of Smoke – FREE Texture by Barbara Courouble. Available at https://www.flickr.com/photos/plumnutz/7856722696/in/photolist-3D1XVu-7QJ4xL-fQb8im-9DvemK-8KGdUq-cYgKW9-7TKDf5-p6CrVD-6meTqN-agyBXN-a2tMaF-5d9M4H-oMWnEK-dMdj2Z-ijBdaF-CqJyt-dPiCM2-aHzyKT-ThKCrH-5Fx1Hg-iNpH9k-2bY121-5wpy8u-64qbTH-kGzfFv-4U48mS-5CDWAC-8MCUGP-daTqKi-kLwRMT-oYnMVT-9M2DUT-njZdQ9-oMtdSN-jAaURw-bpZvVo-6vGnpm-dYtAmP-kGzoTa-oqZAZY-k2FMY1-e7c6Wz-ehp9Et-aEAJPk-kLygsC-9NEtYQ-o1ipRg-drQeLR-c5XXRL-9EbwvZ Licensed under CC BY-NC 2.0
Match by Bastain. Available at https://www.flickr.com/photos/bneumann/2821962797/in/photolist-5inidZ-6ZRk6-DRLd5-tTLsQ-Guvnh-n3Cze-6ZRcF-kmCVBR-wrFWU-4LSs4f-Stv2w8-e4WdZm-hSiuww-wrFTb-8qEyUE-96bp33-8MA2Ho-wrFR7-Fesxw-7FiEgb-oTvg81-9LHYoU-3JAFqN-4FdfTi-5mW5WX-ojMwb3-4NMjAP-ekG8N6-avzjPr-aM9jN-ehdEyD-8yn3xT-8Y8KDk-5ZYN8o-7CYU4u-qkTDS-6CbyhG-9hkQN-6ZQrq-HdcJ81-onzHTC-jJPLs-5inqxi-52sDX8-8qDitT-8PdRik-pXUR2Y-9RjSa-GrAe2g-ox3QH Licensed under CC BY-SA 2.0
Did you Know
Smoking hand rolled cigarettes is just as dangerous as pre-made cigarettes. Indeed, there is evidence to suggest poorer health outcomes in those who roll their own cigarettes.
